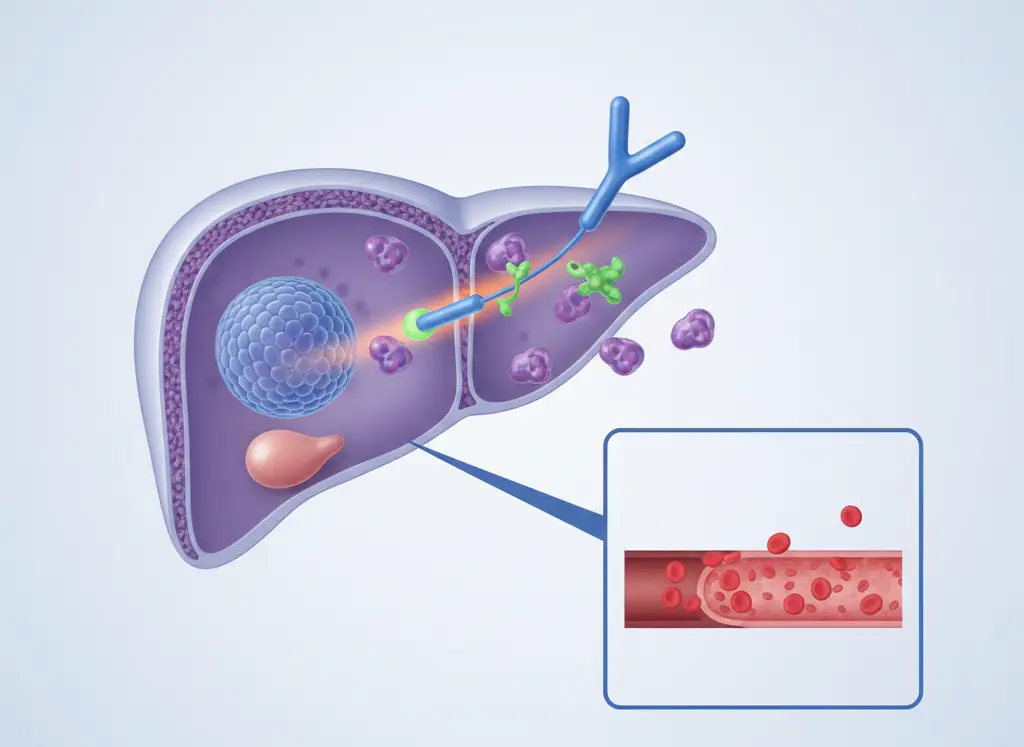
Prostatitis refers to a group of conditions that cause inflammation of the prostate gland. It can lead to symptoms such as pelvic discomfort, urinary difficulties, and pain during or after urination. In some cases, symptoms resolve with treatment. In others, they persist for months or longer.
Understanding why prostatitis becomes chronic in certain individuals requires looking beyond symptoms alone. The underlying cause plays a central role in determining which treatments are effective and which are not.
Prostatitis Includes Several Distinct Conditions
Prostatitis is not a single diagnosis. It includes multiple clinical categories, each with different causes and treatment considerations.
Some forms of prostatitis are caused by bacterial infection and respond well to antibiotics. Others occur without any detectable infection and are classified as inflammatory or chronic pelvic pain syndromes. These non-bacterial forms account for a significant proportion of long-term cases.
Because symptoms can overlap across categories, prostatitis is sometimes treated uniformly despite important biological differences.
Chronic Inflammation Is the Most Common Driver of Persistent Symptoms
In chronic prostatitis, ongoing symptoms are most often associated with persistent inflammation rather than active infection.
An initial trigger such as infection, physical irritation, or urinary reflux may start the process. Over time, even after the original trigger has resolved, inflammatory activity within the prostate can remain elevated.
This ongoing inflammation may:
- irritate prostate tissue
- affect local blood flow
- increase sensitivity of surrounding nerves
- interfere with normal tissue repair
When inflammation becomes self-sustaining, symptoms may continue despite the absence of bacteria.
Why Antibiotics Are Often Ineffective in Chronic Prostatitis
Antibiotics are an appropriate treatment when bacterial infection is present. However, in chronic prostatitis without infection, antibiotics do not address the underlying cause.
Some individuals experience temporary symptom relief during antibiotic treatment. This may be related to secondary anti-inflammatory effects rather than elimination of infection. In many cases, symptoms return once treatment ends.
When inflammation or tissue dysfunction is driving symptoms, infection-focused treatment alone is unlikely to provide lasting improvement.
How to diagnose prostatitis and Its Limitations
Diagnosis typically begins with ruling out serious conditions. Common evaluations include urine testing, prostate-specific antigen (PSA) measurement, physical examination, and imaging when clinically indicated.
These tools are effective for identifying infection, obstruction, or malignancy. They are less effective at assessing chronic inflammatory activity, immune dysregulation, or tissue-level changes within the prostate.
As a result, diagnostic results may appear normal even when symptoms persist. This reflects the limitations of standard testing rather than the absence of disease.
Why Accurate Diagnosis Influences Treatment Outcomes
Treatment decisions are most effective when they align with the underlying cause of symptoms.
- Bacterial prostatitis requires antimicrobial therapy.
- Inflammatory prostatitis may benefit from strategies aimed at reducing inflammation and supporting tissue recovery.
- Pain related to nerve sensitisation may require additional management approaches.
Without identifying the primary driver, the best treatment for prostatitis often involves repeated interventions with limited benefit.
Chronic Prostatitis and Impaired Tissue Recovery
Long-term inflammation can affect how prostate tissue responds to injury and stress. Persistent inflammatory signalling may reduce the prostate’s ability to return to a stable, non-irritated state.
Over time, this can contribute to ongoing discomfort and symptom recurrence. Addressing chronic prostatitis often requires attention to both inflammation and tissue recovery rather than symptom control alone.
A More Targeted Clinical Perspective
UGO Genetics UK focuses on identifying biological factors that contribute to persistent inflammation and impaired healing.
This includes evaluating how inflammatory processes are being regulated and whether the conditions needed for tissue recovery are present. Such approaches are typically considered when standard treatments have not led to sustained improvement.
Key Takeaways
Chronic prostatitis is most commonly driven by unresolved inflammation rather than ongoing infection. When diagnosis focuses only on excluding disease, treatment options may be limited. Identifying the biological factors maintaining inflammation can help guide more appropriate and effective management strategies.